What is a good death?
By Shanna Provost and GDIN members
Although perceptions of a “good death” in Australia may have evolved over time, there are common elements of a good death across various reports and studies.
From a palliative care perspective, a good death can be defined as patient-centred care where the physical, emotional, psychological, social, cultural, ethical and spiritual needs of a person are addressed.
Here at the Good Death Impact Network (GDIN), a group of changemakers working at the forefront of the end-of-life phase, we continually hear these elements that people consider would constitute a good death for them:
Dignity
Comfort (no suffering)
Pain-free (symptom control)
Understanding what is happening and what’s coming next (not for all cultures however[1])
A sense of being in control and being able to make choices (or have someone advocate for them)
Companionship and community (especially if there is no support from loved ones)
Open communication between healthcare providers, patient and family
Being with the right people
Being in the desired environment (not everyone wants to die at home)
Cultural, ethical and spiritual wishes acknowledged and incorporated
Bereavement Care (most people are concerned for their loved ones more than themselves)
The academic review of a good death
According to a systematic review published in The Lancet 2021[2], a good death includes conditions such as dying at the preferred place, relief from pain and psychological distress, emotional support from loved ones, autonomous treatment decision-making, avoiding futile life-prolonging interventions, and not being a burden to others. The review highlighted that the right to end one’s life is a significant factor in enabling control over one’s fate during the final stages of life.
Cultural perspectives
Respecting cultural ideologies comes up often in my work. For example, whilst cultural beliefs vary significantly between communities, in Australian Indigenous cultures, a 'good death' is understood as a process that ensures the safe and respectful passage of the spirit into the afterlife, guided by cultural protocols and ceremonies. This may include the desire to die on Country[3].
The importance of palliative care in a good death
Palliative care is a key element to ensuring that all of these needs are considered and put in place because it supports the emotional and spiritual well-being of patients and their families – promoting inner peace, acceptance of death, and meaningful connections with others. It recognises the importance of companionship, whether from family, friends, or trained professionals like death doulas, and provides access to pastoral or psychological support services. The holistic model of palliative care, which integrates clinical, psychosocial, and spiritual care, aims to improve the quality of life for both patients and caregivers during the final stages of life.
Some still argue that the medical approach to dying needs a reset. “While dying is a normal part of life, death is often treated as an illness[4]. Palliative care focuses primarily on anticipating, preventing, diagnosing, and treating symptoms experienced by patients with a serious or life-threatening illness and helping patients and their families make medically important decisions. The ultimate goal of palliative care is to improve quality of life for both the patient and the family, regardless of diagnosis.”
Studies on a good death
The survey by Coret and Martimianakis[5] also reflects a general consensus on the elements of a good death with a small group of responders feeling that it provided autonomy, better care and less isolation, but interestingly, when surveyed on technology’s role during death, a larger group spoke of prolongation, suffering, less autonomy, less dignity and more distance. Once again, a supportive palliative care team might be able to bridge that gap.
Grattan Institute’s Dying Well report of 2014[6] (Hal Swerissen and Stephen Duckett) says that a good death gives people dignity, choice and support to address their physical, personal, social and spiritual needs.
The Good Death Impact Network perspectives on a good death
Who better to ask about what a good death is, than the people working tirelessly to enable better death outcomes in Australia – the Good Death Impact Network? In this article some of our GDIN members share their perceptions of what constitutes a good death, and their responses show that death is a unique experience for all of us.
“While it is commonly said that most people want to die at home, there are those who feel safe, comfortable and cared-for in a more clinical setting such as a hospital, where their loved ones are free to do nothing other than sit with them and give them their full attention. For us therefore, a ‘good death’ happens when the person dies as they wish, and when they are free of fear”, says Jan McGregor from the Pure Land Home Hospice in Adelaide.
“Following my clinical death, I want my body to be left undisturbed for as long as possible, ideally for three days or until a Buddhist practitioner has determined that my consciousness has left my body”, she says.
Whilst many agree on the key elements for a ‘good death’, there are others who argue that the idea of ‘good death” should be abandoned because it is subjective and raises unrealistic expectations.
Danni Petkovic, Death Doula shares:
“I know many people use the term ‘good death,’ but I do try to avoid language that suggests there’s a right or wrong way. I focus more on a death that aligns with someone’s values.In my worldview, it is not a moment. It’s a continuum of care, honesty, and human connection that reflects who you are. A death shaped by values, not by circumstances. After a year of webinars, workshops, panels, community dinners, screenings, death cafes, conferences and death literacy projects, and supporting our wonderful hosts, I’d summarise the community reflection as: ‘a good death is one where a person is known, heard, and supported, where their choices are honoured, their suffering eased, their community present, and their final days reflect the truth of who they are. It’s not perfect or painless, but it is human, connected, and theirs’.”
Bec Lyons, Independent Funeral Director and Board President of the Australian Home Funeral Alliance tends to agree (as do I).
“To me the notion of a good death is misleading in a way, cause it places value on it and positions some as bad deaths. And to be fair, some deaths are crap. But... to me a good death is an informed one; a death achieved with intentionality and compassion; where the dying person had enough agency to put thought and consideration into their end and make choices that were meaningful, and then had enough conversations with their people that those people felt empowered to carry out those wishes for them, however big or small. That is a good death because it both honours the dead and nourishes the grief of those who live on”, she says.
Joe Sehee, Community companion to the dying from Social Health Australia shares a poignant experience:
“Finding common humanity in death can allow it to move beyond being a personal tragedy so that it can become accepted as a universally-shared experience. When any difficult event occurs, I think that we experience it differently when we know that others are having to deal with the same thing. Sometimes solace can even be found in those moments, which was something I observed while companioning a dying woman, first by herself, and then the following day when she was surrounded by family. While she seemed scared, and almost ashamed when I first met her, this woman seemed like a different person when connected to her loved ones. And that probably had a lot to do with the kinds of things I heard being said that second time I saw her. I’ll never forget her brother telling me, loud enough for his dying sister to hear: “There’s only going to be three of us after she goes. I’ll probably be the one up next.” I looked over at the woman just as a peaceful smile appeared on her face. That was a good death.”
Michelle Chaperon, Founder of Carers’ Circle, a website designed to help people caring for aging parents, has this to say from an adult child perspective:
“A good death, or the ‘ideal’ death for my parents and for me as their adult child, is one where their wishes are known, understood, and lovingly enacted. It means being able to honour who they are and who they’ve been – not only in their final moments, but also in the time leading up to their death, and the way we celebrate their life afterwards.
A good death creates space for stories, laughter, and tears, allowing us to honour them fully and authentically while supporting each other in our grief. For us, it would feel peaceful, deeply loving, and forgiving. It would be free from uncertainty because their choices were openly discussed – where we were making decisions about their care to enable their wishes, rather than having to make the decisions ourselves”, she says.
Of course, we’ve been speaking about what constitutes a good death when a terminal prognosis has been determined, but we don’t only die from terminal illness. Other leading causes of death include land transport and other accidents, suicide, accidental poisoning, SIDS, strokes, heart attacks, and death at the hands of others[7].
That’s why I (Shanna Provost, Author of the Rest Easy Journal and End-of-Life Education Specialist) focus on helping people to get their affairs in order long before death knocks at the door, because honestly, we just don’t know what’s around the corner.
So for me, I don’t think in terms of a ‘good’ death, but of a ‘graceful’ death. What’s the difference? A graceful death means that I have set in place and discussed everything that will help my loved ones to either journey with me through a terminal prognosis or be able to process what is required after I die, no matter how it happens because I have taken the time and commitment to put my affairs in order.
How the Good Death Impact Network is creating change
As part of its mission to create change and improve outcomes for everyone when someone dies, the Good Death Impact Network’s playbook outlines how we can do this from a systems perspective.
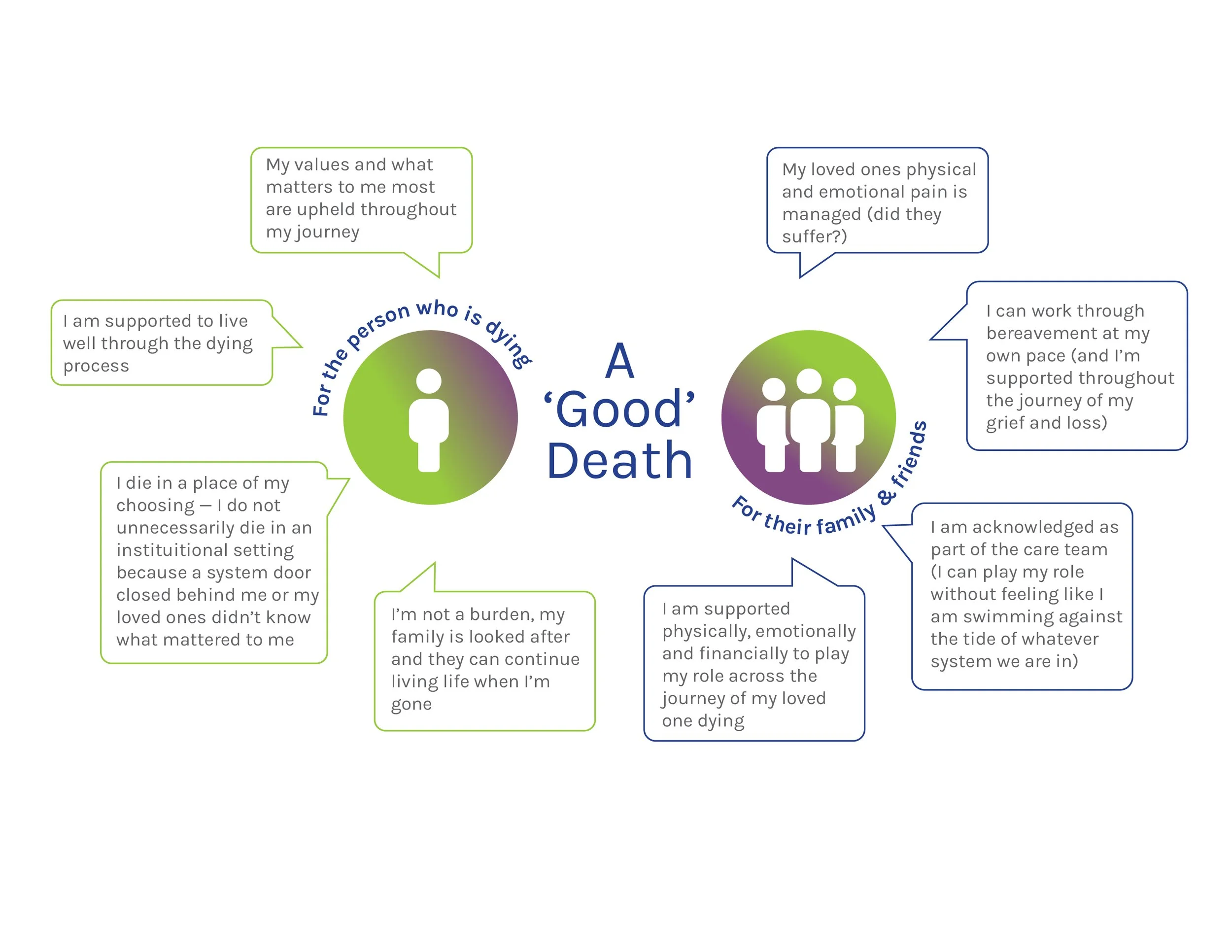
But the most important element of systems are people – so in our work we consider both the person who is dying and their family and friends. This diagram drives our work.
How do you feel about this? What do you think makes a good death? We’d love to hear from you. Join us in a conversation on LinkedIn, or get in touch.
_____________________________________________________________________________________________________________________________
[1] Some cultures, such as Filipino and South East Asian cultures, do not openly talk about death and dying and do not wish for patients to be told they are dying due to their cultural beliefs, but it’s equally important not to make assumptions based on a patient’s culture.
[2] What would it take to die well? A systematic review of systematic reviews on the conditions for a good death https://www.thelancet.com/journals/lanhl/article/PIIS2666-7568(21)00097-0/fulltext
[3] https://www.creativespirits.info/aboriginalculture/people/mourning-an-aboriginal-death
[4] The Role of Palliative Care at the End of Life, Oschner Journal https://www.ochsnerjournal.org/content/11/4/348
[5] Wiley Health Science Reports, https://onlinelibrary.wiley.com/doi/full/10.1002/hsr2.1374
About the author: Shanna Provost
As a Funeral Celebrant, specialist educator in end-of-life issues and Death Doula (trained by Dr Michael Barbato), Shanna's passion is to encourage people to think about, discuss and make clear their choices about the end of their natural life.
Shanna's Rest Easy Journal and Rest-Easy Toolkit are sold across Australia. These gentle, easy-to-follow tools guide people to get their affairs in order and leave clear information for those left to sort everything after they have died.
Shanna is a Good Death Impact Network Member.

